Atopic dermatitis, also known as eczema, is a chronic inflammatory skin disease condition causing visible rashes, pain, burning, and itching—sometimes unrelenting, maddening itching.
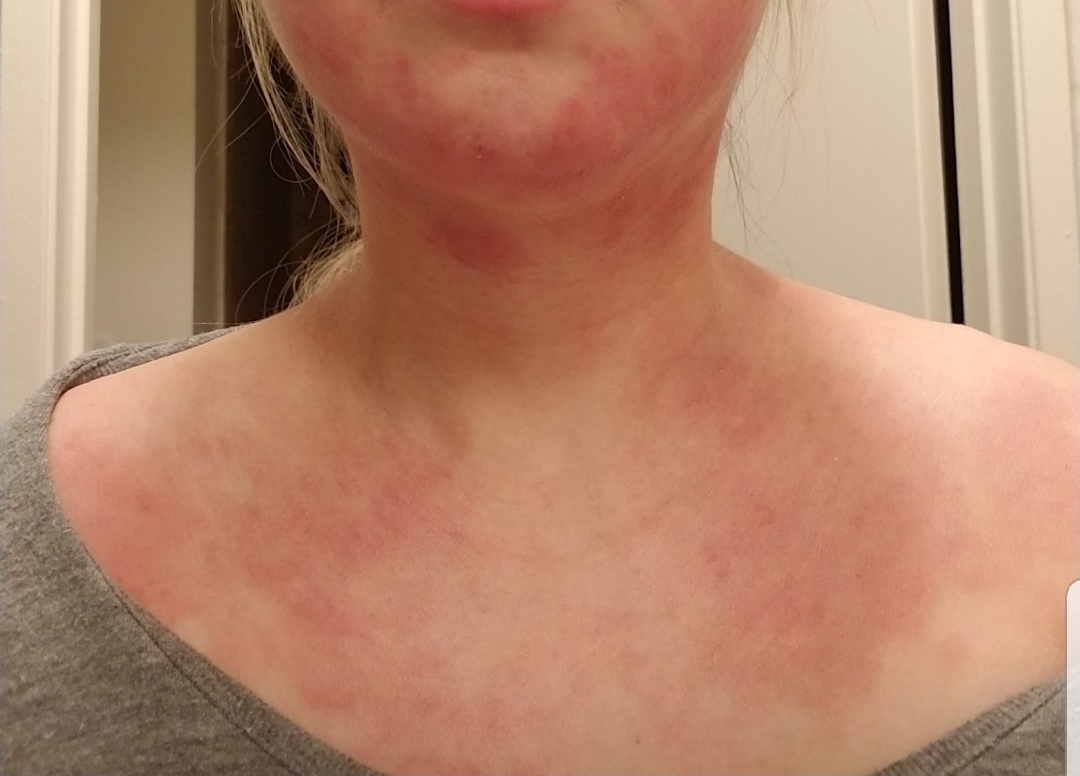
Dermatologists have long known that bad cases of the condition were also associated with numerous psychiatric issues, including depression and anxiety. In addition, children with eczema perform worse in academics and adults with the condition do worse at work and have fewer job opportunities compared to healthy peers.
Yet the extent of the psychiatric burden had not been fully appreciated until recently, when USC researchers conducted a meta-analysis of 15 published clinical studies that evaluated psychiatric issues associated with atopic dermatitis—including issues of suicidality.
What they found was surprising even to veteran dermatology providers: patients with atopic dermatitis were 44 percent more likely to experience suicidal thoughts and 36 percent more likely to attempt suicide than the general population.
Patients may suffer from the condition for months or years, and sometimes caregivers can provide little relief, particularly from the itching.
"When you talk to patients, they describe the itching as absolutely miserable—an intensity of nine out of ten, all the time, across large areas of the body. We're starting to get better tools to control itching, but it's still a difficult issue for many," said principal investigator April W. Armstrong, MD, MPH, Department of Dermatology, of the Keck School of Medicine of USC. "We knew patients with atopic dermatitis can get very distressed, but the meta-analysis gave us a much more accurate understanding of just how serious these psychiatric issues were."
The study, "Association Between Atopic Dermatitis and Suicidality: A Systematic Review and Meta-analysis," was published in JAMA Dermatology, in November of 2018. Along with Armstrong, authors were Jeena K. Sandhu, BA; Kevin K. Wu, BA; Thanh-Lan Bui, MA.
The link between eczema and suicidality is not well-understood. The obvious physical and psychosocial burdens likely contribute, as well as the sleep loss caused by the itching, wrote the authors. Additionally, the increased levels of proinflammatory cytokines associated with atopic dermatitis may alter serotonin metabolism, disrupting the balance of neurotransmitters. But more research is needed to understand the potential role of cytokines.
The role of statistical modeling in meta-anaylses.
The 15 studies Armstrong and her team included in their meta-analysis included approximately 4.7 million participants, of which more than 310,000 were atopic dermatitis patients. The analysis aimed to measure rates of suicidal ideation, attempts, and completed suicides.
To extract meaningful insights from multiple and varied studies involving such a large number of participants meant that the research team had to be certain their statistical models and math were solid.
"Meta-analyses can be particularly complicated because you're looking at different populations, from different studies, and attempting to draw larger conclusions," said Armstrong. "So we have to be careful to ensure that the model we're using is adequate and that our conclusions are valid."
For assistance, the team turned to the SC CTSI's Biostatistics, Epidemiology and Research Design (BERD) Core group, directed by Wendy Mack, PhD.
Clinical investigators often focus on biostatistics to help inform study design, or to understand results or impact of an intervention, explained Armstrong. But in a complex meta-analysis, statistical modeling is the investigators' most important research tool.
This was clearly the case in the eczema meta-analysis. "We had specific questions in our study and the biostatistics consultants were instrumental in making sure our findings were valid," said Armstrong. "Dr. Mack and the biostatistics team helped us synthesize the literature and its data, and guided us in our effort to quantify the risk of suicidality across a wide array of studies. And from those findings we were able explain to public the surprising psychological burden of this disease."
Fortunately, the majority of atopic dermatitis patients have mild to moderate symptoms. But for the 20 to 30 percent with moderate or worse cases—nearly 2 million patients—the findings suggest physicians should keep psychiatric concerns in mind when evaluating patients with serious cases of atopic dermatitis. "It is important for dermatology providers to be aware of this increased risk in patients with atopic dermatitis, monitor for suicidality, and make appropriate referrals to mental health professionals," wrote the study's authors.
